Welcome to FVI
Both nursing students and healthcare organizations rave about FVI.
Our commitment is to enabling students to do great things in healthcare and working with top healthcare employers in South Florida. Our team is dedicated to understanding student and partner needs. FVI works to ensure students learn and practice the vital skills for them to be successful in a healthcare career. We also scour the community to identify and partner with top healthcare organizations for both curriculum development and graduate employment placement. Specific curriculums, expert educators, modern facilities and sim labs, and a personalized focus ensure our students have an optimized experience.


Is a Healthcare Career Right for You?
Take the Healthcare Career Readiness Quiz
Identify goals, personal strengths and important facts about your potential career path so you can make an informed decision about your future. It takes just a few minutes!Get Your Healthcare Career Readiness Score Now!
Healthcare Programs
Join FVI for the opportunity to safely learn the essential skills for high demand healthcare careers. FVI School of Nursing and Technology prepares students to become healthcare professionals as Nurses, Medical Assistants, Pharmacy Technicians, Patient Care Technicians, and Nursing Assistants.


Assoc. of Science in Nursing
The Associate of Science in Nursing (ASN) program offered at FVI School of Nursing prepares...
Details
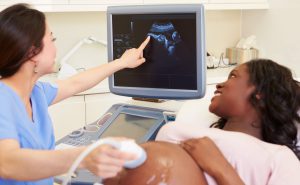

DMS
The DMS (Ultrasound) program teaches students to use ultrasound to produce diagnostic images that assist health...
Details


Medical Assistant
The Medical Assistant program is designed to train students in all of the relevant aspects of medical office ...
Details


Pharmacy Technician
This program provides instruction in how to assist the pharmacist in the packing and distribution of medication...
Details


Health Services Admin.
The Health Service Administration (HSA) program prepares students for entry-level administrative positions in outpatient...
Details
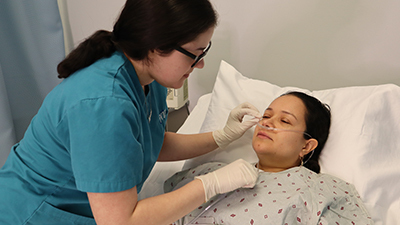

Patient Care Technician
Our Patient Care Technician program provides you with technical medical career skills that focus on patient care...
Details
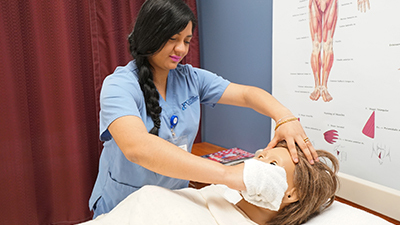

Home Health Aide
Our Home Health Aide program is designed to offer students an understanding of patient care...
Details


Medical Office Admin
An associates degree will be awarded upon completion of the medical office administration program.
Details














